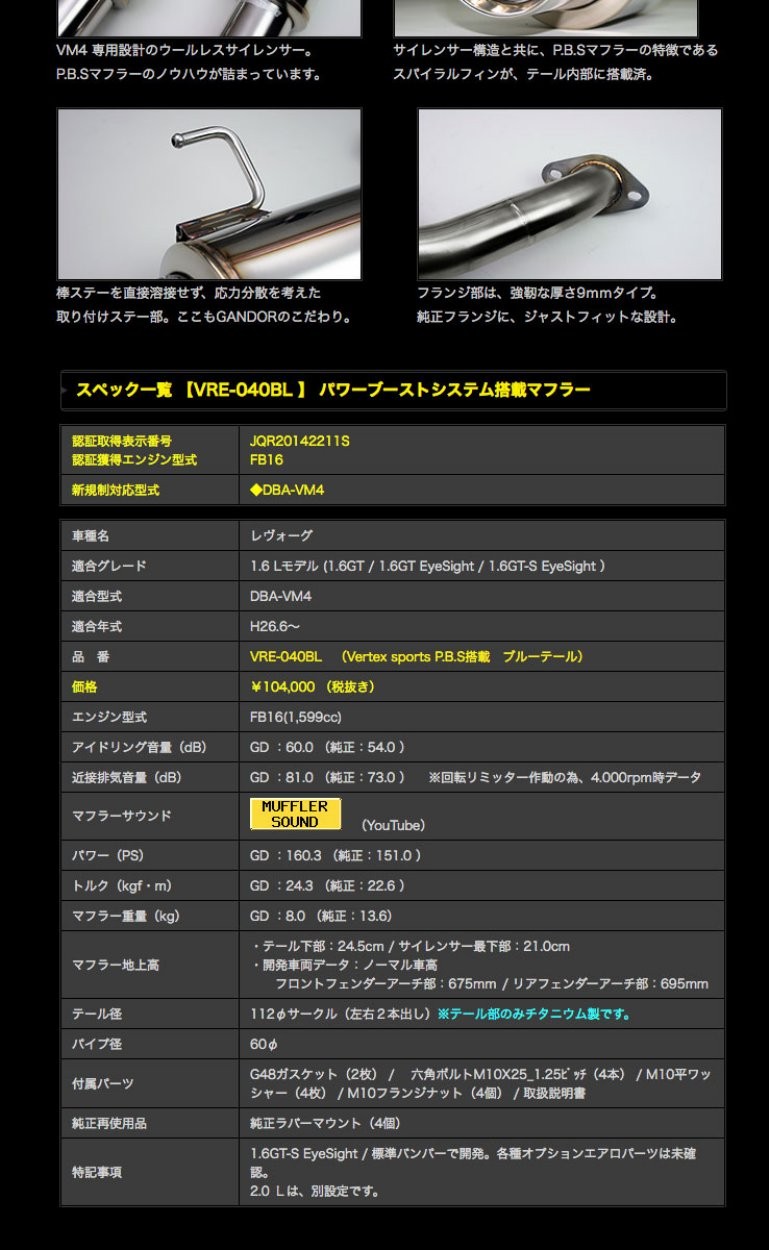
GANADOR マフラー Vertex sports スバル レヴォーグ DBA-VM4 H26/6〜 品番:VRE-043TP受注生産 ガナドール【沖縄・離島発送不可】
(税込) 送料込み
商品の説明
商品情報
メーカー:GANADOR (ガナドール)
127512円GANADOR マフラー Vertex sports スバル レヴォーグ DBA-VM4 H26/6〜 品番:VRE-043TP受注生産 ガナドール【沖縄・離島発送不可】車、バイク、自転車自動車Amazon.co.jp: GANADOR (ガナドール) 【ガナドール チタンマフラー
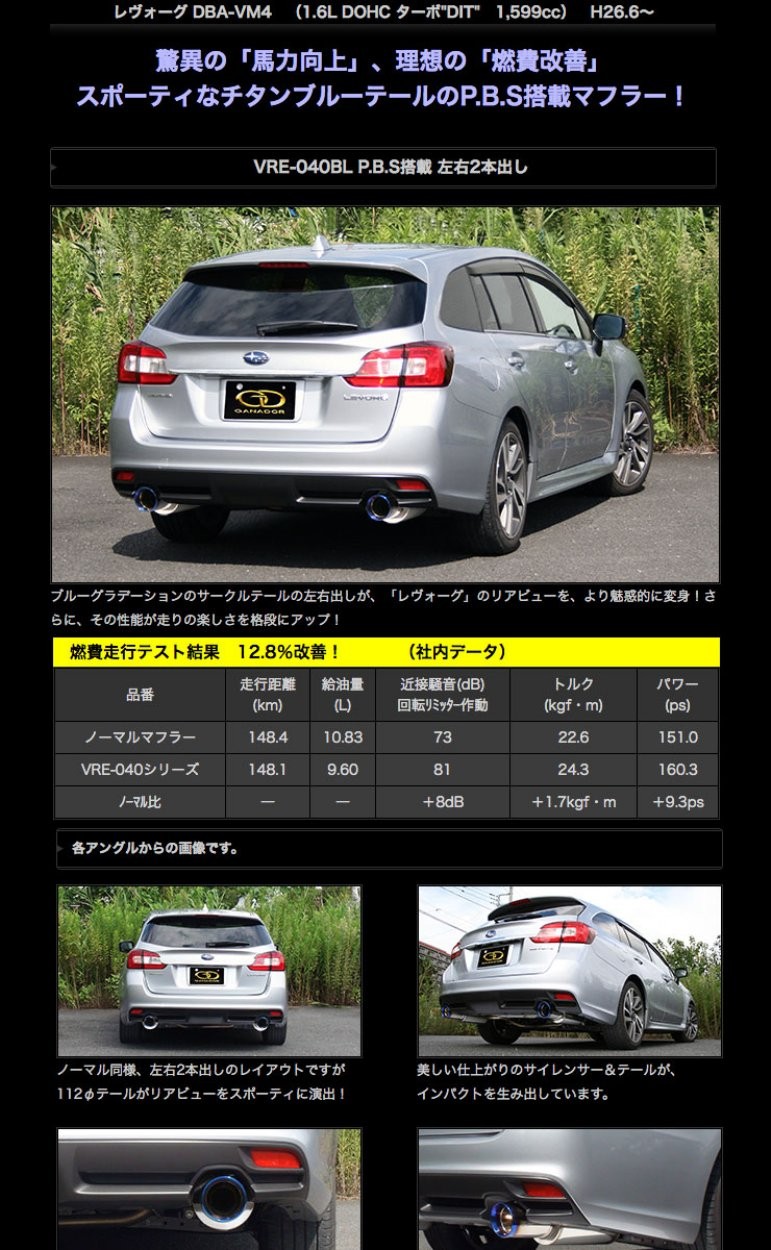
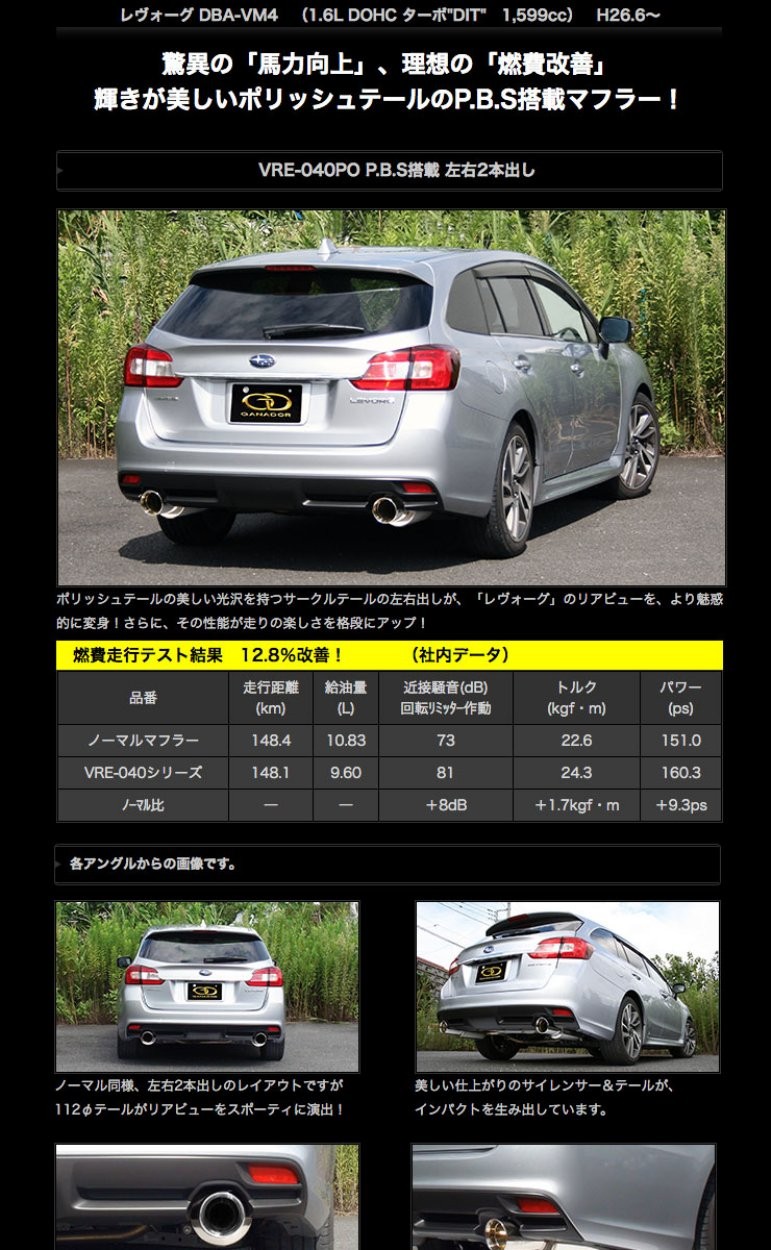
商品名:Vertex sports (バーテックス スポーツ)
品番:VRE-043TP
材質/テールカラー:オールチタン製/ポリッシュ仕上げ
テール径(φ)/出口形状:112/左右2本出し サークル
認定:JQR
●適合車種:スバル レヴォーグ
●車両型式:DBA-VM4
●エンジン型式:FB16
●年式:H26/6〜
●注意事項:完全受注生産品。センターパイプ付フルサイズマフラー 標準バンパー専用 1600cc
◇適合詳細につきましては、メーカーホームページも必ずご確認ください。
送料 全国一律 5,500円(税込)
※ただし、沖縄県・離島へは発送できません。ご注文いただいた場合はキャンセルさせていただきます。
※大型商品につき、配達日指定及びお時間指定はできません。
※一部受注生産品がございます。必ず事前に納期をお問い合わせください。
※画像は全車種共通で使用しております。車により商品形状が異なる場合があります。GANADOR マフラー Vertex sports スバル レヴォーグ DBA-VM4 H26/6〜 品番:VRE-040PO ガナドール【沖縄・離島発送不可】
GANADOR マフラー Vertex sports スバル レヴォーグ DBA-VM4 H26/6
□GANADOR ガナドールマフラー VM4 レヴォーグ チタンテール 砲弾
取付店への発送で送料無料 GANADOR ガナドール マフラー Vertex sports H26/6〜 DBA-VM4 レヴォーグ (個人宅・沖縄離島は別途送料) : p363908 : フジ スペシャルセレクション - 通販 - Yahoo!ショッピング
□GANADOR ガナドールマフラー VM4 レヴォーグ チタンテール 砲弾
ガナドール PBS.S搭載 マフラー レヴォーグ DBA-VM4 VRS-040PO GANADOR
VRE-043PO | GANADOR
□GANADOR ガナドールマフラー VM4 レヴォーグ チタンテール 砲弾
□GANADOR ガナドールマフラー VM4 レヴォーグ チタンテール 砲弾
ガナドール PBS.S搭載 マフラー レヴォーグ DBA-VM4 VRS-040PO GANADOR
取付店への発送で送料無料 GANADOR ガナドール マフラー Vertex sports H26/6〜 DBA-VM4 レヴォーグ (個人宅・沖縄離島は別途送料)
ガナドール PBS.S搭載 マフラー レヴォーグ DBA-VM4 VRS-040PO GANADOR
VRE-043TBL/VRE-043TPO | GANADOR
□GANADOR ガナドールマフラー VM4 レヴォーグ チタンテール 砲弾
ガナドール 車用マフラー レヴォーグの人気商品・通販・価格比較
□GANADOR ガナドールマフラー VM4 レヴォーグ チタンテール 砲弾
ガナドール 車用マフラー レヴォーグの人気商品・通販・価格比較
Amazon.co.jp: GANADOR (ガナドール) 【ガナドール チタンマフラー
ガナドール PBS.S搭載 マフラー レヴォーグ DBA-VM4 VRS-040PO GANADOR
ガナドール 車用マフラー レヴォーグの人気商品・通販・価格比較
ガナドール 車用マフラー レヴォーグの人気商品・通販・価格比較
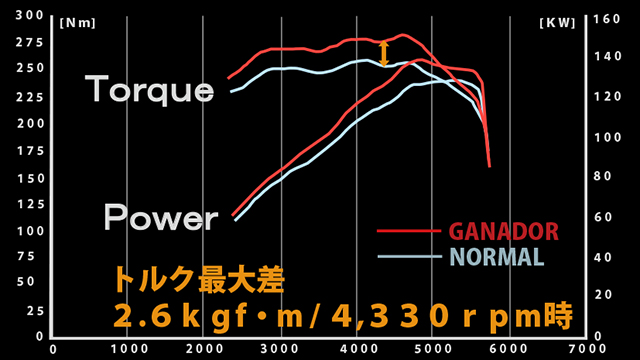
【ガナドール公式】 レヴォーグ1.6 VM4 ノーマル比較 マフラーサウンド VRE-047PO(リヤピース) 純正オプション リヤバンパースカート用
ガナドール PBS.S搭載 マフラー レヴォーグ DBA-VM4 VRS-040PO GANADOR
Amazon.co.jp: GANADOR (ガナドール) 【ガナドール チタンマフラー
ガナドール 車用マフラー レヴォーグの人気商品・通販・価格比較
VRE-043PO | GANADOR
Amazon.co.jp: GANADOR (ガナドール) 【ガナドール チタンマフラー
VRS-052BL | GANADOR
ガナドール 車用マフラー レヴォーグの人気商品・通販・価格比較
VRE-053BL | GANADOR
ガナドール 車用マフラー レヴォーグの人気商品・通販・価格比較
【ガナドール公式】 レヴォーグ VM4/VMG マフラー商品説明 標準バンパー用 VRE-040/-041/-042/-043シリーズ
ガナドール公式】 レヴォーグ 1.6L VM4 マフラーサウンド VRE-040
GANADOR ガナドール Vertex Sports P.B.S搭載 左右4本出し サークル
GDS-420BL | GANADOR
ガナドール PBS.S搭載 マフラー レヴォーグ DBA-VM4 VRS-040PO GANADOR
ガナドール PBS.S搭載 マフラー レヴォーグ DBA-VM4 VRS-040PO GANADOR
ガナドール 車用マフラー レヴォーグの人気商品・通販・価格比較
Amazon.co.jp: GANADOR (ガナドール) 【ガナドール チタンマフラー
ガナドール公式】 レヴォーグ1.6 VM4 ノーマル比較 マフラーサウンド
商品の情報
メルカリ安心への取り組み
お金は事務局に支払われ、評価後に振り込まれます
出品者
スピード発送
この出品者は平均24時間以内に発送しています